- HOME
- For Patients
- Vascular insufficiency pain
Vascular insufficiency pain
- About
vascular insufficiency pain - Diagnosis of
vascular insufficiency pain - Treatment of
vascular insufficiency pain - Spinal Cord Stimulation Therapy
Spinal Cord Stimulation Therapy
History of spinal cord stimulation therapy
Spinal cord stimulation therapy has a long history, having been used in countries other than Japan since around 1960. It was first used in Japan from around 1970, and fully implantable generators have been covered by health insurance since 1999. Internationally, generators are implanted in around 20,000 people every year, but in Japan, they have only been used in about 5,000 people, and domestic awareness of this method is low. Recent developments and advances in treatment devices have improved their safety and decreased the burden on patients, and the number of individuals undergoing this treatment in Japan is increasing.
Principles
If the nerve controlling a blood vessel is in a state of high tension, the vessel constricts, and pain occurs at the same time. Spinal cord stimulation alleviates this state of high nervous tension, returning the vessel to its relaxed state. This also has a pain-relieving effect.
Effect
If drug treatment and vascular reconstruction produce little improvement, spinal cord stimulation therapy may be performed to improve blood flow and relieve pain, and may ultimately help avoid outcomes such as the amputation of fingers or toes.
International studies have shown that incorporating spinal cord stimulation therapy is more effective than drug treatment alone in relieving pain and improving blood flow. Vascular insufficiency pain is a condition in which patients suffer from poor blood flow and pain simultaneously. For patients who want to resolve both of these issues, those in whom blood flow has improved somewhat but who would like to eliminate the pain or restore even better blood flow, spinal cord stimulation therapy may provide the answer. When small vessels in the arms and legs are involved, it may also be difficult to insert a device from inside the blood vessel. Spinal cord stimulation therapy is considered for the treatment of the nerve controlling small vessels in locations such as these. At our hospital, this treatment is offered collaboratively by specialists in circulatory medicine, cardiovascular surgeons, plastic surgeons, anesthesiologists and foot care nurses.
Limitations
Spinal cord stimulation therapy is effective in only a limited number of cases. It is not necessarily effective against all types of pain and ischemia. Furthermore, even when it does work, its effectiveness may decline with long-term use or if the skin has already become dark and discolored. Spinal cord stimulation therapy is not effective against pain due to psychological or social factors such as stress and social factors.
Practical use of spinal cord stimulation surgery
Around one week of hospitalization is required. Patients who are taking blood-thinning medication before admission will need to discontinue this medication temporarily.
Patients are admitted to hospital on the day before surgery and undergo the operation the following day.
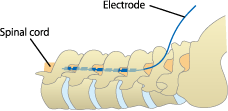
Surgery is carried out under local anesthesia with the patient lying face down. A needle is inserted into the lower back, and an electrode is slowly inserted through this needle into the epidural space (the space around the dura mater, a protective membrane that covers the spinal cord). X-ray imaging is used to check the distance and direction in which the electrode is advanced. The electrode is soft and about 1.3 mm in diameter. A stimulus is applied to the spinal cord from this electrode to create a tingling sensation at the same site where the pain is felt or ischemia is present, which is identified during surgery by asking the patient to place the electrode in the ideal spot.
Once the position of the electrode has been decided, a generator is implanted. This generator is small and is implanted in a fatty area such as the flank or buttocks. After the generator has been implanted, it can be adjusted from outside the body. The stimulation method is adjusted while observing the patient's sensations and skin color to see whether the blood flow has improved, with the aim of relieving pain and restoring blood flow. The generator can be controlled externally by the patient, who is told how to operate the generator once the current, voltage, and other conditions have been determined.
The current that flows from the generator after implantation is very weak, meaning that there is no possibility of it causing an electric shock or noise. Furthermore, this current does not exert any control over the patient's own actions or emotions. The implantation site may be a little hard, and it may be possible to feel a bump.

Site of electrode implantation
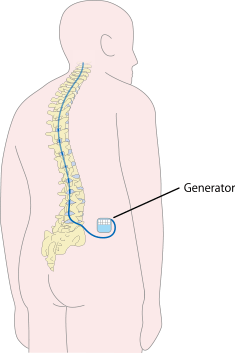
Generator implantation
Complications
The electrode is inserted on the outside of the dura mater membrane covering the spinal cord, but because the electrode is a foreign body inside the patient, a rejection reaction, infection, or other reaction may appear. The large number of blood vessels at the electrode insertion site means that bleeding may also occur. If bleeding is severe, it may compress the spinal cord or nerves and cause damage. Potential mechanical malfunctions include broken wires and the electrode slipping out of position. These complications are extremely rare, but they do occasionally occur, and the doctor in charge will provide a full explanation before surgery.
Postoperative lifestyle
Patients are asked to avoid vigorous exercise for a short time after the operation, but before long they can return to their everyday lifestyle without restrictions. The doctor in charge will instruct patients who were taking blood-thinning medication when they can start taking the medication again. Patients who have undergone spinal cord stimulation therapy can operate the generator themselves, and they should make their own adjustments in accordance with how severe the pain is. They should consult their doctor about the degree of improvement of blood flow, as evidenced by skin color, and adjust the generator accordingly. Once they have become accustomed to the stimulation, they can also adjust their medication in consultation with the doctor in charge.
The implanted generator may cause MRI scanners used to diagnose disease to malfunction. Today, devices other than MRI scanners can be used for diagnosis, so the first thing is to tell the doctor that you have had a generator implanted. If necessary, doctors will communicate with each other to discuss how this can be dealt with. Some devices that can be used with MRI scanners have become available since January 2014.
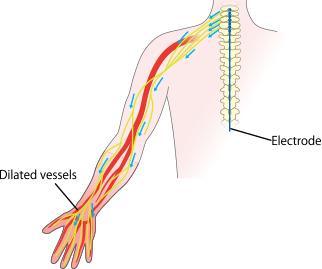
Dilated blood vessels

Decreased pain
Generator replacement
The generator for spinal cord stimulation therapy contains a battery. (Some types contain an internal battery and others a rechargeable battery.) This runs down as a result of continued everyday electrical stimulation and may require replacement. The frequency with which the battery must be replaced varies depending on the type of generator implanted and the stimulation conditions. Details are given during the explanation provided before surgery.
Notes
Spinal cord stimulation therapy is not the “last hope Efor chronic pain and for ischemia. We are unable to treat patients for whom all other forms of treatment have failed and who are looking to try it as a last resort.
Before surgery, it is impossible to tell which nerve controls which blood vessel, and how many remaining vessels there are for which blood flow improvement is actually feasible. Even with the best treatment plan, it is not always possible to relieve pain completely or prevent the amputation of fingers or toes.
A key feature of spinal cord stimulation treatment is that patients are able to vary the intensity of stimulation and other factors for themselves in accordance with the severity of their pain. This means that patients who are unable to adjust their generator themselves, such as those suffering from dementia, cannot be considered for this treatment.